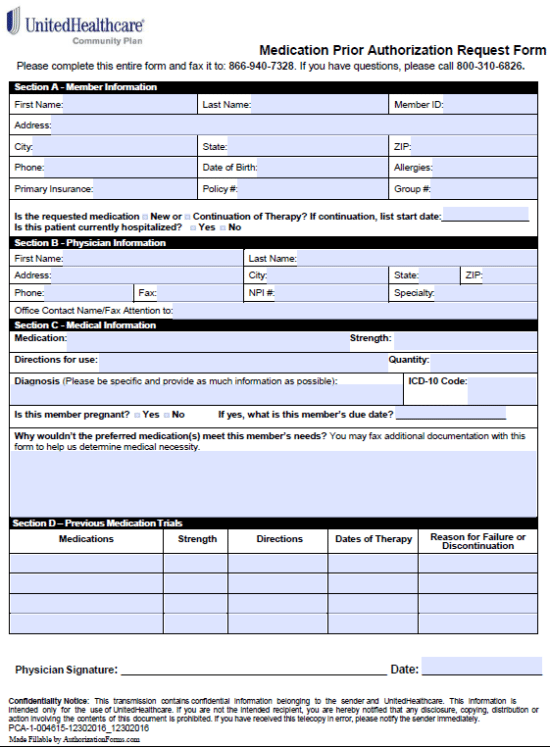
Preauthorization Form - Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process set by many insurance. Your health insurance or plan may require preauthorization for certain services. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Sometimes called prior authorization, prior approval or precertification. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific.
Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process set by many insurance. Your health insurance or plan may require preauthorization for certain services. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Sometimes called prior authorization, prior approval or precertification. Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided.
Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Your health insurance or plan may require preauthorization for certain services. Sometimes called prior authorization, prior approval or precertification. Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process set by many insurance. Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements.
United Healthcare Prior Authorization Form 2023 Pdf Printable Forms
Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Your health insurance or plan may require preauthorization for certain services. Sometimes called prior authorization, prior approval or precertification. Preauthorization is a process that.
FREE 8+ Sample Prior Authorization Forms in PDF MS Word
Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Sometimes called prior authorization, prior approval or precertification. Your health insurance or plan may require preauthorization for certain services. Preauthorization (p.a), also known as precertification, prior.
FREE 41+ Authorization Forms in PDF Excel MS word
Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Your health insurance or plan may require preauthorization for certain services. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process.
FREE 13+ Prior Authorization Forms in PDF MS Word
Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Your health insurance or plan.
FREE 8+ Sample Travel Authorization Forms in PDF MS Word
Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process set by many insurance. Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Sometimes called prior authorization, prior approval or precertification. Your health insurance or plan may require preauthorization for certain services. Insurance companies and health plans use prior.
Simply prior authorization form Fill out & sign online DocHub
Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Sometimes called prior authorization, prior approval or precertification. Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process set.
Fillable Online AUTHORIZATION AGREEMENT FOR PREAUTHORIZATION Fax Email
Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Sometimes called prior authorization, prior approval or precertification. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Your health insurance or plan may require preauthorization for certain services. Modernizing.
Humana Prior Authorization Request Form Fill and Sign Printable
Sometimes called prior authorization, prior approval or precertification. Preauthorization (p.a), also known as precertification, prior authorization, or prior approval is a mandatory process set by many insurance. Your health insurance or plan may require preauthorization for certain services. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Modernizing.
Humana Prescription Drug Plan Prior Authorization Form
Sometimes called prior authorization, prior approval or precertification. Your health insurance or plan may require preauthorization for certain services. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Preauthorization.
FREE 13+ Prior Authorization Forms in PDF MS Word
Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Your health insurance or plan may require preauthorization for certain services. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided. Sometimes called prior authorization, prior approval or precertification. Preauthorization (p.a), also known as.
Preauthorization (P.a), Also Known As Precertification, Prior Authorization, Or Prior Approval Is A Mandatory Process Set By Many Insurance.
Your health insurance or plan may require preauthorization for certain services. Modernizing the prior authorization process, this program is available for provider groups meeting eligibility requirements. Preauthorization is a process that occurs before treatment, where healthcare providers obtain approval from the insurance company for specific. Insurance companies and health plans use prior authorization to make sure that a specific medical service is necessary and being provided.